Digestion and Nutrient Absorption
Understanding how the digestive system breaks down food, absorbs nutrients, and the role of the microbiome in digestive health.

Overview of the Digestive System
The digestive system comprises the mouth, esophagus, stomach, small intestine, large intestine (colon), and accessory organs (liver, pancreas, gallbladder). This system's purpose is breaking down food into component nutrients, absorbing those nutrients, and eliminating waste.
Digestion involves both mechanical processes (chewing, muscular contractions) and chemical processes (enzymatic breakdown). The time food spends in the digestive system (transit time) typically ranges from 24-72 hours, though individual variation is substantial and depends on food composition, hydration status, physical activity, and individual factors.
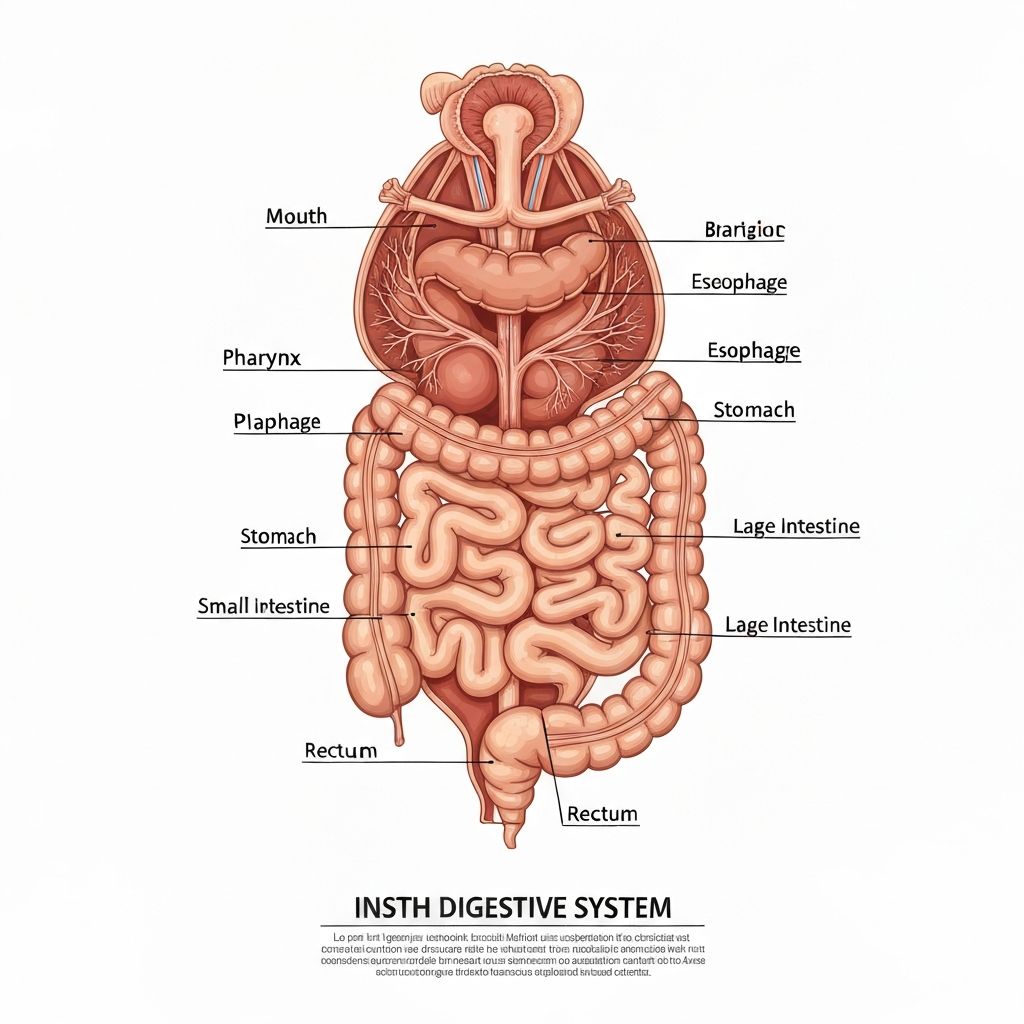
Stages of Digestion
Mouth and Esophagus
Digestion begins in the mouth where mechanical breakdown occurs through chewing and enzymatic breakdown begins with salivary amylase (which breaks down starch). Saliva also lubricates food, facilitating swallowing and beginning carbohydrate digestion. The food bolus travels down the esophagus through peristalsis (muscular contractions) to the stomach.
Stomach
The stomach is a muscular organ that contracts to mechanically break down food into smaller particles (chyme). The stomach secretes gastric acid (hydrochloric acid) and the enzyme pepsin, which begins protein breakdown. Gastric acid also kills many bacteria in food and provides an acidic environment necessary for optimal enzyme function.
Stomach acid is protective and necessary for digestion, despite its reputation as problematic. The stomach protects itself from acid through mucus secretion. Food typically remains in the stomach 2-4 hours, though this varies substantially based on food composition and individual factors.
Small Intestine
The small intestine (duodenum, jejunum, ileum) is the primary site of nutrient absorption despite being relatively small in diameter. The small intestine receives chyme from the stomach along with pancreatic digestive enzymes and bile from the gallbladder.
Pancreatic enzymes include amylase (breaks down remaining starch), proteases (break down proteins), and lipase (breaks down fats). Bile emulsifies fats, enabling lipase to break down fat molecules. The small intestine's epithelium has specialized cells with microvilli that dramatically increase surface area for absorption—approximately 30 square meters of absorptive surface in a relatively small organ.
Nutrient absorption in the small intestine includes glucose and amino acids (via active transport), fatty acids and fat-soluble vitamins (via diffusion after incorporation into micelles), and various minerals. Different nutrients are absorbed in different regions of the small intestine.
Large Intestine (Colon)
The colon receives undigested material and water. Primary functions include water absorption, electrolyte absorption, and fermentation of undigested material by bacterial microbiota.
The Microbiome and Digestive Health
The human gastrointestinal tract harbors approximately 100 trillion microorganisms—primarily bacteria, along with archaea, fungi, and viruses. This microbial community, termed the microbiome, plays crucial roles in digestive health, immune function, and metabolic regulation.
The microbiome is not static but responds to dietary patterns, medications (particularly antibiotics), stress, sleep, and other lifestyle factors. This plasticity offers opportunities for dietary interventions to support beneficial microbial populations.
Functions of the Microbiome
Fermentation and Short-Chain Fatty Acid Production
Microbiota ferment undigested carbohydrates (particularly fiber) to produce short-chain fatty acids (SCFAs): butyrate, propionate, and acetate. These SCFAs are crucial—butyrate serves as the primary fuel for colon epithelial cells, propionate influences liver metabolism, and acetate enters systemic circulation.
SCFAs have anti-inflammatory properties, support intestinal barrier integrity, influence satiety through interactions with appetite-regulating hormones, and may influence metabolic health. This mechanism explains why adequate fiber intake is associated with health benefits beyond simple mechanical bowel function.
Vitamin Synthesis
Some B vitamins (particularly B12, though bioavailability is limited) and vitamin K are synthesized by gut bacteria. While the degree to which microbiota-derived vitamins contribute to systemic requirements is debated, this synthesis represents an important additional function of the microbiome.
Immune Function
The microbiome educates and regulates the immune system. Specific bacterial metabolites (particularly butyrate) influence regulatory T cell development, reducing excessive immune activation. The microbiome also produces antimicrobial compounds that suppress pathogenic bacteria.
Intestinal Barrier Function
The intestinal epithelium forms a barrier preventing translocation of bacterial lipopolysaccharides and undigested food antigens into circulation. Certain bacteria produce compounds that strengthen tight junctions between epithelial cells, enhancing barrier function.
Metabolism and Energy Harvest
Microbiota fermentation of dietary fiber yields additional calories beyond direct macronutrient absorption. The degree to which different microbiota compositions influence energy harvest from identical diets remains an active area of research.
Factors Supporting Digestive Health and Microbiome Diversity
- Dietary fiber: Prebiotic fiber (soluble fiber from oats, legumes, vegetables, fruits) feeds beneficial bacteria and supports SCFA production.
- Fermented foods: Foods like yogurt, kefir, sauerkraut, and tempeh contain beneficial bacteria and compounds that support microbiota diversity.
- Diverse plant foods: Different plant foods feed different bacterial populations. Greater food diversity supports greater microbiota diversity.
- Whole grains: Provide fiber and resistant starch that feed beneficial bacteria.
- Polyphenol-rich foods: Compounds in tea, coffee, berries, and other plants serve as substrates for bacterial fermentation and have antimicrobial properties.
- Adequate hydration: Supports normal bowel function and nutrient absorption.
- Physical activity: Exercise influences microbiota composition and diversity.
- Sleep quality: Sleep deprivation disrupts microbiota composition and function.
- Stress management: Chronic stress alters microbiota composition; stress-reducing practices support healthy microbiota.
- Judicious antibiotic use: While necessary for treating bacterial infections, unnecessary antibiotic use disrupts microbiota and may have lasting effects.
Individual Digestive Variation
Digestive capacity, transit time, and food tolerance vary significantly between individuals. Lactose tolerance, gluten sensitivity, food allergies, and various digestive disorders reflect individual differences in digestive function and immune response to specific foods.
These variations underscore that optimal dietary composition requires individual assessment rather than universal prescriptions. A food that is well-tolerated and supports digestive health in one individual may be problematic for another.